Welcome to Central Chiropractic Clinic
Chiropractic Services & Treatments
Coventry Chiropractors, Physiotherapy & Pain Clinic
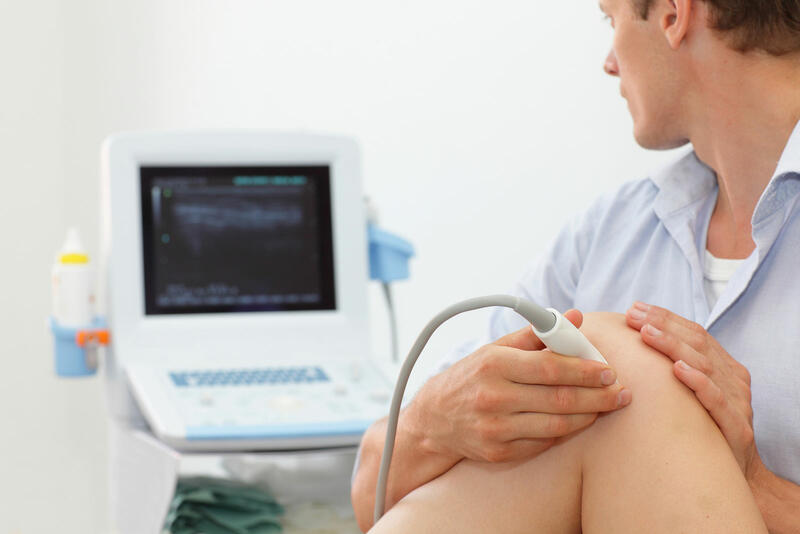
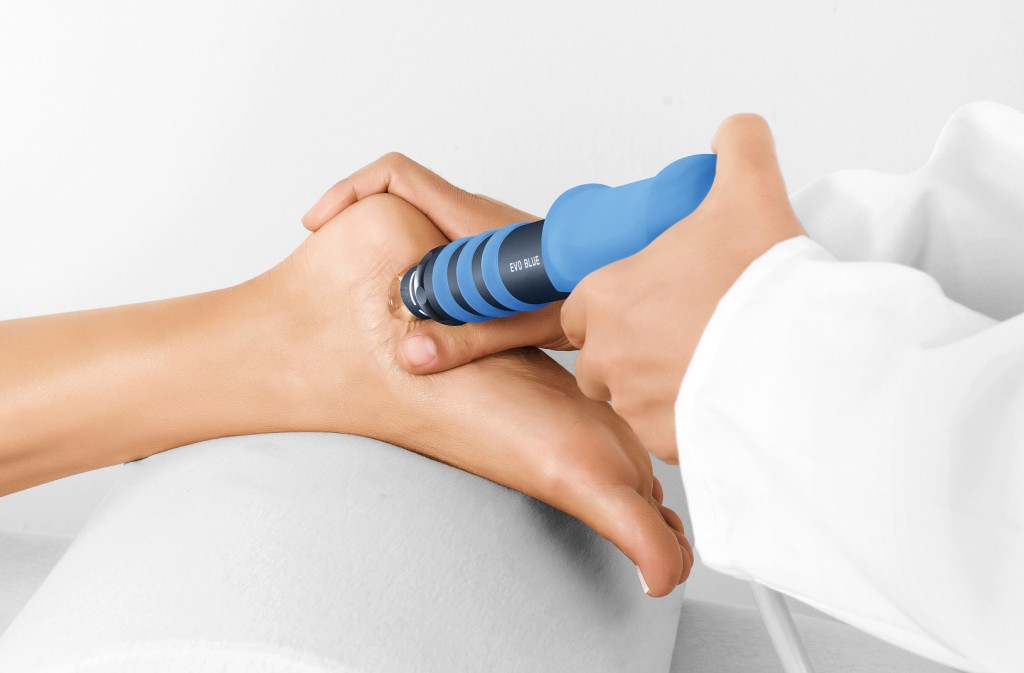
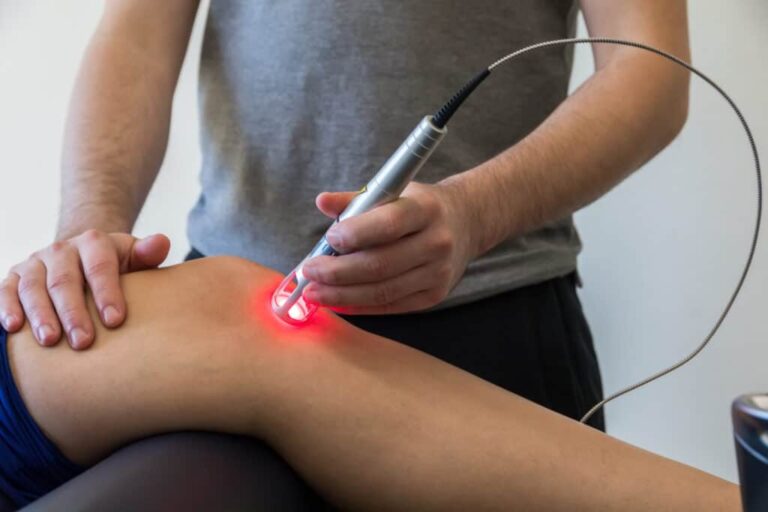
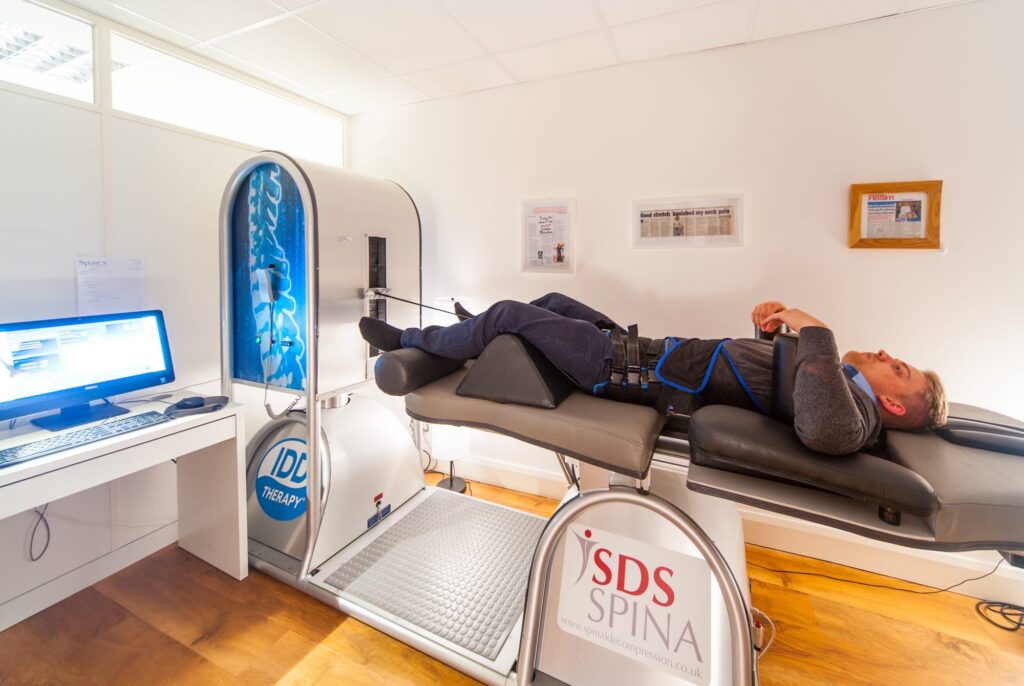
Our specialist modalities called IDD Therapy, Shockwave Therapy, K- Laser Therapy, Digital X-rays, Diagnostic Ultrasound Scans – provide professional pain relief which is non-invasive or surgical, eliminating the need for anaesthesia or injections.
IDD Therapy, Extracorporeal Shockwave Therapy and K- Laser Therapy are proven successful in treating acute and chronic pain conditions including trapped nerves, sciatica, RSI and recurrent injuries, tendinopathies, bursitis, Achilles tendinitis, and other painful conditions affecting hip, knee, ankle, heel and foot joints.
Our expert knowledge, outstanding customer service and top quality professional standards have made it to the top 3 highly rated Chiropractors in Coventry, UK.
Professional Pain Relief treatment and complete service dedicated to helping ease your pain. Your chiropractor will not only understand the pain you are suffering with, but they will be committed to devising the right course of treatment to remedy it.
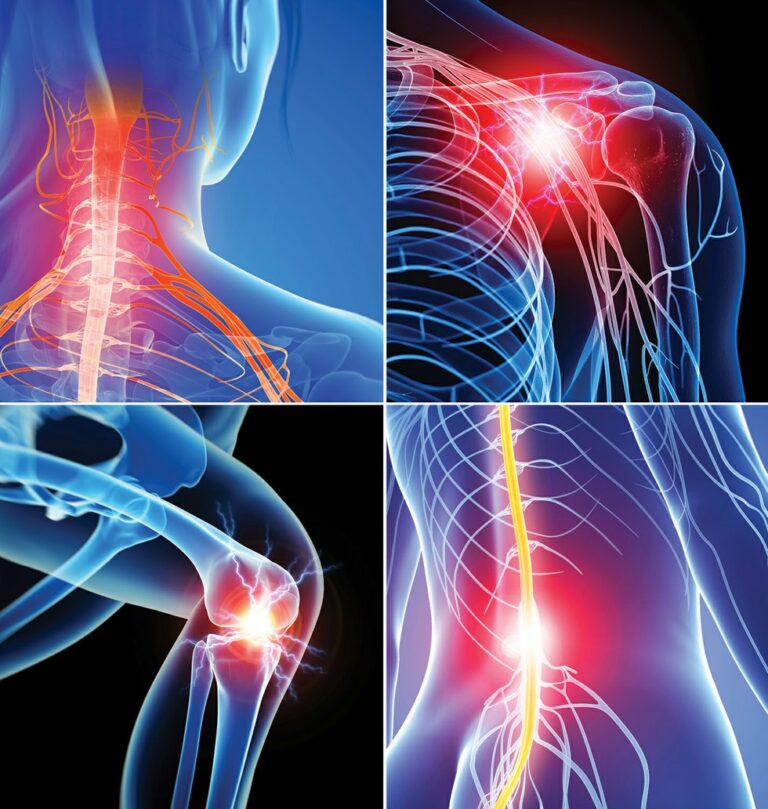
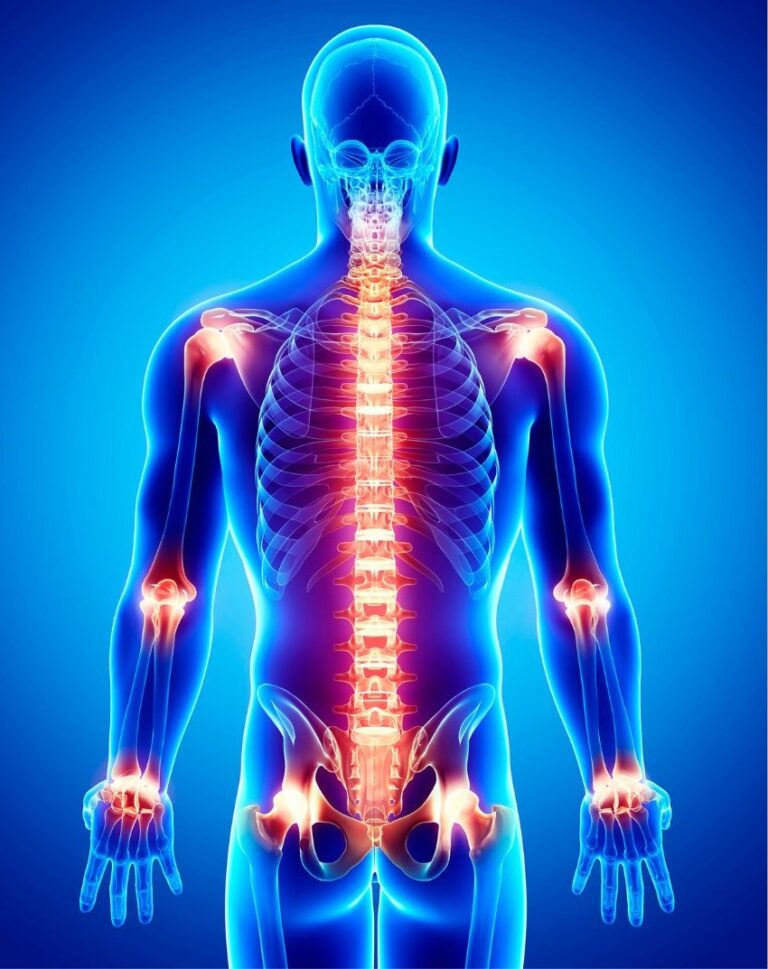
Your chiropractor will be able to help you manage the various types of pain caused, such as Back Pain, Neck and Shoulder Pain, Headaches, Leg Pain, Arm Pain, Back Injuries, Sciatica etc.
Welcome to Central Chiropractic and Physiotherapy Clinic including Coventry Back Pain Clinic. CV1 2LD. For decades we have been helping the people of Coventry, Leamington Spa, Warwick, Nuneaton, and Rugby, to manage and overcome a wide range of injuries and conditions.
Our team of fully qualified and registered chiropractors and physiotherapists in Warwickshire and the West Midlands can assess and treat you in our state of the art clinic.
Each chiropractor is registered with The British Chiropractic Association (BCA) and The General Chiropractic Council (GCC) and has a minimum of 4 or 5 years of full-time education and training – assuring you that they can offer you the right course of pain relief for your specific problem.
Diagnostic Ultrasound scans and Digital X-rays provide accurate diagnostic assessments.
We are recognised by leading healthcare insurers.
Central Chiropractic Clinic does not except BUPA Health insurance
Private Health Insurance Terms and Conditions
We also offer an HPC registered physiotherapy for Back Pain, Diagnostic ultrasound scanning, Digital X-rays service at the clinic.
Specialist modalities used include:
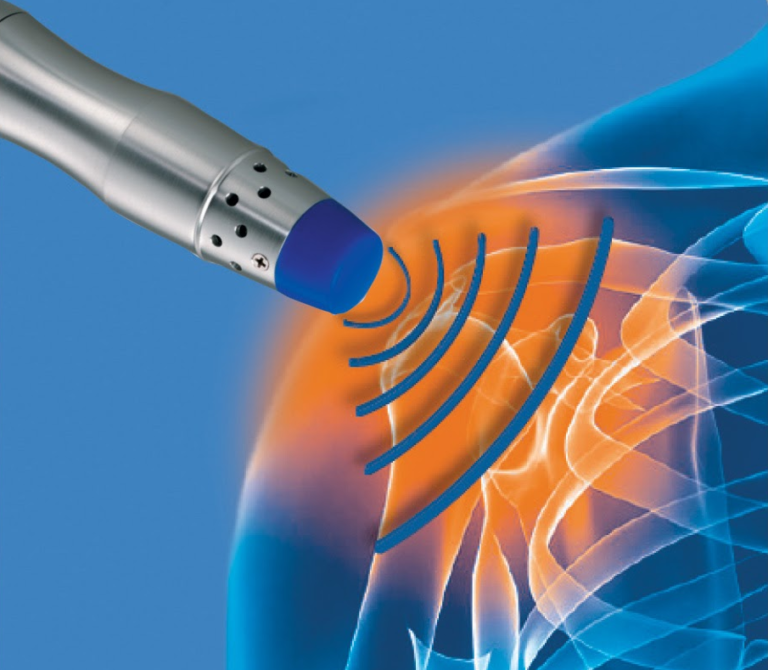
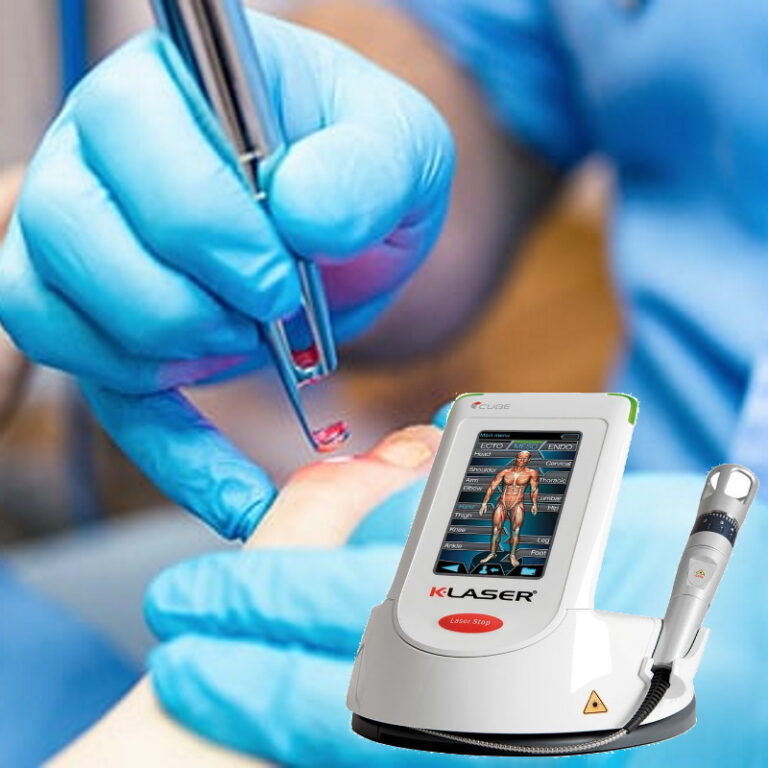
IDD Therapy, both Focused and Radial Shockwave Therapy, Medical K-Laser Therapy are proven successful in treating chronic and recurrent injuries and conditions.
Central Chiropractic Clinic provides IDD therapy, Shockwave therapy and K-Laser Therapy are recommended and used by neurosurgeons and orthopaedic surgeons and consultants.

What our patients say










GET IN TOUCH
Tel: 02476 222002
Email: info@centralchiropracticclinic.co.uk
Address: 12 Park Road, Coventry, Warwickshire, CV1 2LD
CLINIC HOURS
Monday – Friday: 7:30am – 7pm
Saturday: 8am – 1pm
Accreditors